Measles in Aotearoa New Zealand - current locations of interest
How do you catch measles?
Measles is highly contagious and spreads through the air by coughing, sneezing, saliva, mucus, or by touching an infected surface. It can survive for up to two hours in the air. A person with measles is most contagious from when symptoms start until three to four days after the rash appears.
Who is at risk of catching measles?
- Anyone who has not had two doses of a measles vaccine after 12 months of age
- Anyone who has not had measles before
Most people born in Aotearoa New Zealand before 1969 are immune to measles. This is because before that time almost everyone had measles as a child.
Measles can lead to serious complications, including:
- Ear infections, which can cause permanent hearing loss
- Diarrhoea
- Pneumonia
- Swelling of the brain – this is rare, but can cause permanent brain damage or death.
Symptoms
It takes about 10-12 days for your child to develop symptoms after being in contact with someone with measles.
The first symptoms of measles are similar to the cold or flu, so it may be hard to tell it is measles.
Early symptoms may include:
- Fever
- Cough
- Runny nose
- Sore and watery pink eyes (conjunctivitis)
- Small white spots on the back inner cheek of the mouth (called Koplik spots).
Day 3-7 symptoms may include:
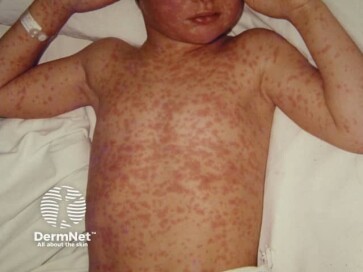
- A rash that starts on the face, behind the ears, and moves over the head and down the body. It can look like pink or red spots or bumps and is not usually itchy. The rash can last a week or more.
If your child has measles symptoms
- Stay home. Don’t go to work or send your child to day care or school to prevent the spread of infection
- Call PlunketLine on 0800 933 922 or your doctor to check if your child needs to be seen
- Don't go to your doctor's clinic without phoning first, because measles can spread easily to others in the waiting room.
What does measles rash look like? (credit: DermNet)

If you or someone in your whānau has measles
If you or someone in your whānau are diagnosed with measles, your local Public Health Service will contact you to give you advice and support. Public Health staff will let you know what you need to do to keep yourself, your household members and the community safe while you recover.
Tamariki with measles can be very unwell and need lots of care. There’s no specific antiviral treatment for measles once symptoms start, but hospital care (when needed) can help to manage severe complications.
How to protect your child
- Check your child’s MMR (measles, mumps, rubella) vaccination status. If they have not had the MMR vaccine and are 12 months or older, get them vaccinated.
- Children usually receive their MMR vaccinations at 12 months and 15 months. It's important to get vaccinated on time – but it's never too late to catch up.
- Parents of infants less than 12 months who are travelling overseas or may be at high risk of exposure can talk to their GP. In some cases, an MMR vaccine before 12 months (MMR dose 0) may be recommended. This requires a prescription and tamariki will still need the usual scheduled MMR doses at 12 months and 15 months.
- Make sure you and the rest of your whānau have had two doses of the MMR vaccine. Ensuring the entire whānau is immunised against measles is particularly important to pretect pēpi less than 12 months
- If you are born before 1969, you are considered to have immunity. People born after that date need to have had two doses for full immunity. If you are unsure, there is no harm in getting an extra MMR vaccine dose.
Measles Immunisation Facts
- Immunisation is the only way to prevent measles.
- It's FREE for all tamariki and most adults.
- Plunket offers MMR vaccines at 20 clinics around Aotearoa for the whole whānau: pēpi (from 12 months), tamariki, rangatahi, and adults.
- You can also visit your local pharmacy or medical centre for vaccination.
- Two doses of the measles vaccine provides the most effective protection for you, your family and the wider community. After one dose of the MMR vaccine, about 95% of people are protected from measles. After two doses, more than 99% of people are protected.
- If you're unsure whether your child has been immunised, or you can't find your records, you can check with your Well Child Tamariki Ora provider, or contact your family doctor.
- If you're still unsure, it's safe to get vaccinated again with two more doses.
You can watch health videos like this one in a range of other languages here
Measles and pregnancy
Most pregnant people are already immune through a previous MMR vaccination. If you're not sure if you've been immunised, check your records in your Well Child Tamariki Ora or Plunket book, or ask your family doctor.
People who are pregnant should not get the vaccine.
Pregnant people who catch the measles during pregnancy are at risk of miscarriage, premature (early) labour and having babies with low birth weight. If you are pregnant and know you have encountered someone who has confirmed measles, you should discuss this immediately with your prenatal carer or doctor.
Find out the many ways immunisation benefits you, your tamariki, your whānau, and your community.
Measles and international travel plans
The Ministry of Health strongly recommends that all travellers to any international destination are vaccinated against measles at least two weeks before they travel.
Some Pacific islands including American Samoa, the Republic of Marshall Islands and the Solomon Islands are requiring travellers to show evidence they've been vaccinated against measles at least two weeks before arrival. It is also important you carry documented proof of vaccination or evidence of immunity with you. This may include medical records, laboratory tests, immunisation record summaries, or letters from your GP.
In New Zealand, children receive their first MMR dose at 12 months and their second dose at 15 months as part of the National Childhood Immunisation Schedule.
However, infants aged from six months who are travelling to an outbreak area should have one dose of MMR at least two weeks before they go. Please note that any child vaccinated before 12 months of age will still need two further doses of MMR in line with the National Childhood Immunisation Schedule.
People who are not immune, have symptoms of measles or who have been in contact with someone who has measles in the last 14 days should not travel.
Last reviewed: 3 November 2025